 
The median base curve for RGP lenses was 7.57, and median diameter was 10.00 mm. The mean trial time for attempted eyes (i.e., patients with PMCD who successfully underwent the contact lens trials) was 77.7 minutes, and the number of trials required to finalize the choice of contact lenses ranged between 2 and 7. The average astigmatism was -8.56D, and a majority of the patients with PMCD who were in the contact lens trial had an against-the-rule astigmatism (63.3%). 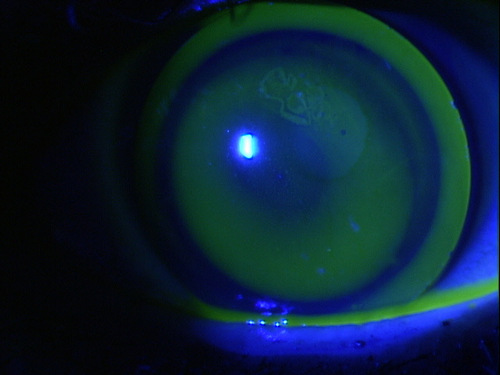
Best-corrected visual acuity of 6/12 or better with spectacles was achieved in 14 (46.66%) eyes. Twenty-seven eyes of 15 patients were identified as subjects for multiple contact lens trials, and 24 (88.8%) eyes were successfully fitted with RGPCLs. There were 12 men and 3 women, with a mean age of 39.73 years. During follow-up, visual acuity with RGPCLs, lens fit, and average wearing time were noted.įifteen patients (30 eyes) with typically inferiorly located pellucid marginal corneal degeneration were included in this study. After successful contact lens trials, data regarding number of trials, trial time, final contact lens choice parameters, and best-corrected contact lens visual acuity were noted for each patient. Twenty-seven of 30 eyes were subjected to several contact lens trials using polymethylmethacrylate (PMMA) contact lenses, using a systematic and consistent approach. Information collected from the medical records included patient demographic data, uncorrected visual acuity, refraction, best-corrected spectacle visual acuity, and topographic details, including kerotometry. This retrospective study consisted of 15 patients with clinical PMCD, confirmed by videokeratography (TMS-1, Computed Anatomy, Inc., New York, NY). Figure 1.To study the clinical performance of rigid gas permeable contact lenses (RGPCL) in patients with pellucid marginal corneal degeneration (PMCD). 5 We, again, would urge the use of a full limbal-to-limbal corneal thickness map to augment other clinical measurements to properly diagnose true PMD. 5 The distinction is not just of academic interest, as treatments such as CXL, intrastromal corneal ring segments, or deep anterior lamellar keratoplasty, which may be appropriate for the more common inferior KCN, would not only be more difficult to perform but may have very different outcomes in true PMD, in which the pathology typically extends past the areas of treatment offered by these modalities. Both inferior keratoconus and PMD are noninflammatory corneal thinning ectatic diseases, but it is important to accurately distinguish these 2 conditions considering the prognosis and overall clinical differences. The vertical Scheimpflug image, however, between these two conditions can be remarkably similar and would fail to differentiate true PMD from inferior keratoconus ( Figure 1). 1 in their article acknowledge the limitations of relying solely on curvature patterns and add a comparison of the superior with inferior corneal thickness taken from the vertical Scheimpflug image. 3,4 Our previous work suggested that a full pachymetric map is a more definitive method to differentiate PMD from inferior keratoconus. Crab-claw patterns on curvature maps are a pattern also seen in the much more common inferior keratoconus. Both of these articles use similar criteria to define PMD, namely inferior corneal thinning and a crab-claw pattern on anterior curvature topography. 2 appeared concurrently in another journal describing the positive results of transepithelial phototherapeutic keratectomy followed by CXL in PMD. 1 advocates for the use of corneal crosslinking (CXL) as a potential treatment of pellucid marginal degeneration (PMD). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
